hi there 👋
I hope everything is well.
I saw two studies last week, highlighting common misconceptions of heart rate variability (HRV) and its applied use, hence I will take this opportunity to write a few considerations about how we can use HRV.
In particular, the misconceptions I am referring to are the following
HRV as a health marker
deep breathing as a tool to increase HRV
In both cases, I think there is a bigger issue with using HRV as a goal metric to improve.
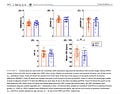
In the first study, "Resting heart rate but not heart rate variability is associated with the normal-weight obesity phenotype" the authors show how resting heart rate, not HRV, is associated with body fat in adults with normal-weight obesity (vs adults that are normal-weight lean). You can find the full text of the paper here, but I have copied the relevant figure below:
This is actually good news as you have much greater control over your resting heart rate, e.g. through exercise, than you have over your HRV (we have shown this multiple times in our work, when it comes to the relationship between e.g. HRV, heart rate and VO2max or other markers of cardiorespiratory fitness, heart rate is much more useful to track changes in fitness than HRV is).
In the second study, "Psychophysiological Effects of Slow-Paced Breathing on Adolescent Swimmers’ Subjective Performance, Recovery States, and Control Perception" the authors report no change in baseline HRV with deep breathing practice. Full text of the paper, here, but again, the relevant table is copied below.
Deep breathing practice improves a number of aspects, typically assessed subjectively (in other studies, anxiety, sleep quality, etc. in this study, cognitive appraisals and biopsychosocial states), but does not necessarily improve baseline HRV (i.e. HRV measured in the morning or the night, not during practice).
This is also not really new, but more evidence is needed, and I suspect there is a lot of individual variability, and also there are a lot of confounders, hence control groups and proper studies are needed here to better capture possible changes and why some people might benefit and others not.
How should we use HRV then?
HRV has a strong genetic component, meaning that it might be hard or not possible to change it over time, especially if we are already reasonably healthy.
The goal, in my opinion, should not be to increase HRV, but to use HRV to improve outcomes that do matter, e.g. our health (and performance, if that's something we care about).
Keep in mind that there is even seasonality in the metrics, so if you start a healthy habit as you approach winter, and your health does improve but your HRV doesn't, it would be really foolish to drop the habit because the metric did not improve (or the other way around, to start any random habit as you approach summer, and then think that the habit is what is causing the change in HRV, while it is just seasonality in many cases). Chronic changes are really hard to analyze, and almost impossible to link causally as we lack a control group.
Using HRV as a feedback loop, to avoid or recover from periods of negative acute stress responses, so that we don't get into a chronically stressed state, is how HRV can be helpful.
It's about relative changes with respect to our normal range, not absolute values.
Examples are: using HRV to determine when to stress more or less the system. This is easy in the context of exercise: e.g. modifying training intensity based on the data, but it can be harder for other stressors (e.g. work or family-related).
However, there is typically room for adjustments, e.g. an extra nap, or eating better, or going for a walk, or making some changes here and there that can help keep the data more stable, which is typically associated with better outcomes.
Achieving stability in HRV might be a more realistic and helpful way to use the data, as opposed to increasing its value (when does increasing it even end? it is obviously a game that can only end at a certain point, what then?).
Needless to say, if there is large room for improvement in our life, e.g. we never exercised or have a really stressful job, making a change, will likely impact the data. Because that change will impact almost any parameter we can measure in our body. Nothing special about HRV under those circumstances (your heart rate will be lower, your glucose levels will be lower, your blood pressure will be lower, your blood markers will be better, etc.
Aim for stability, and keep in mind stability doesn't mean a lack of stress, it means a quick recovery from stressors, if you measure your HRV according to best practices (another reason to ignore real-time HRV monitors, which would give you the false impression that all stress is bad, by measuring too close to the stressor, as opposed to measuring your response after a few hours, the way you do when assessing HRV in the morning).
I hope this provides some useful context about this often misunderstood (and misused) metric.
Don't set yourself up for failure by having unrealistic expectations about how your behavior should change this metric, use it to your advantage to improve the outcomes that matter.
Practical guidelines
In short, here is how I would operate:
1. use a tool that allows you to capture your response (i.e. to measure your HRV) in a repeatable context, far from stressors and confounding factors. That's the morning before you do anything else. If the morning is not practical, the night is an acceptable, though not ideal, option (despite what wearables try to convince you of).
2. use a tool that provides you with your normal range. Most changes in day-to-day data are irrelevant and within normal variability. Only changes outside our normal range should be potentially used to make adjustments: by definition, these are rare occasions.
Once you have those two elements, you can try to add as much context as possible, and try to see what stressors create instability or suppressions below your normal range, and what you can do about it.
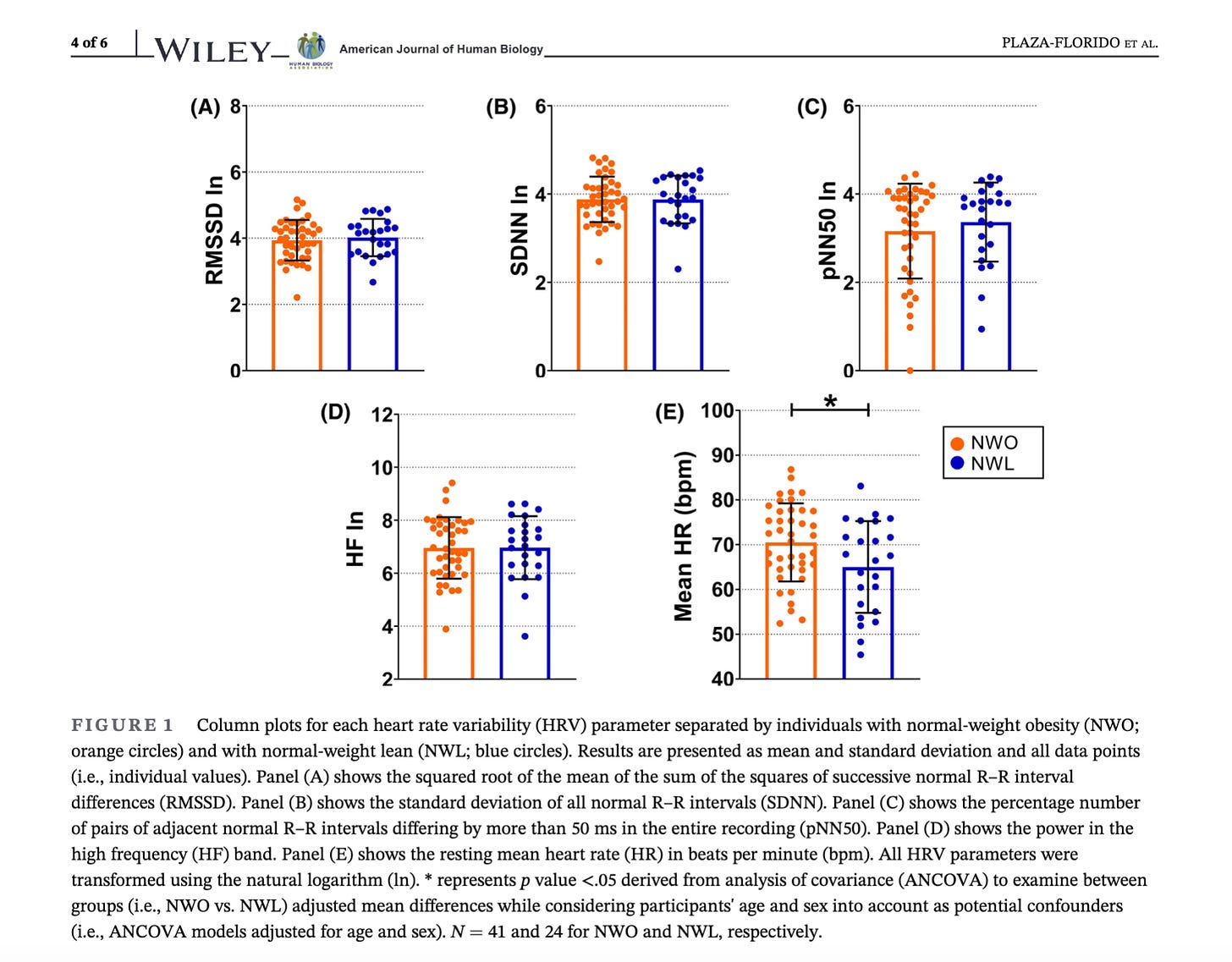
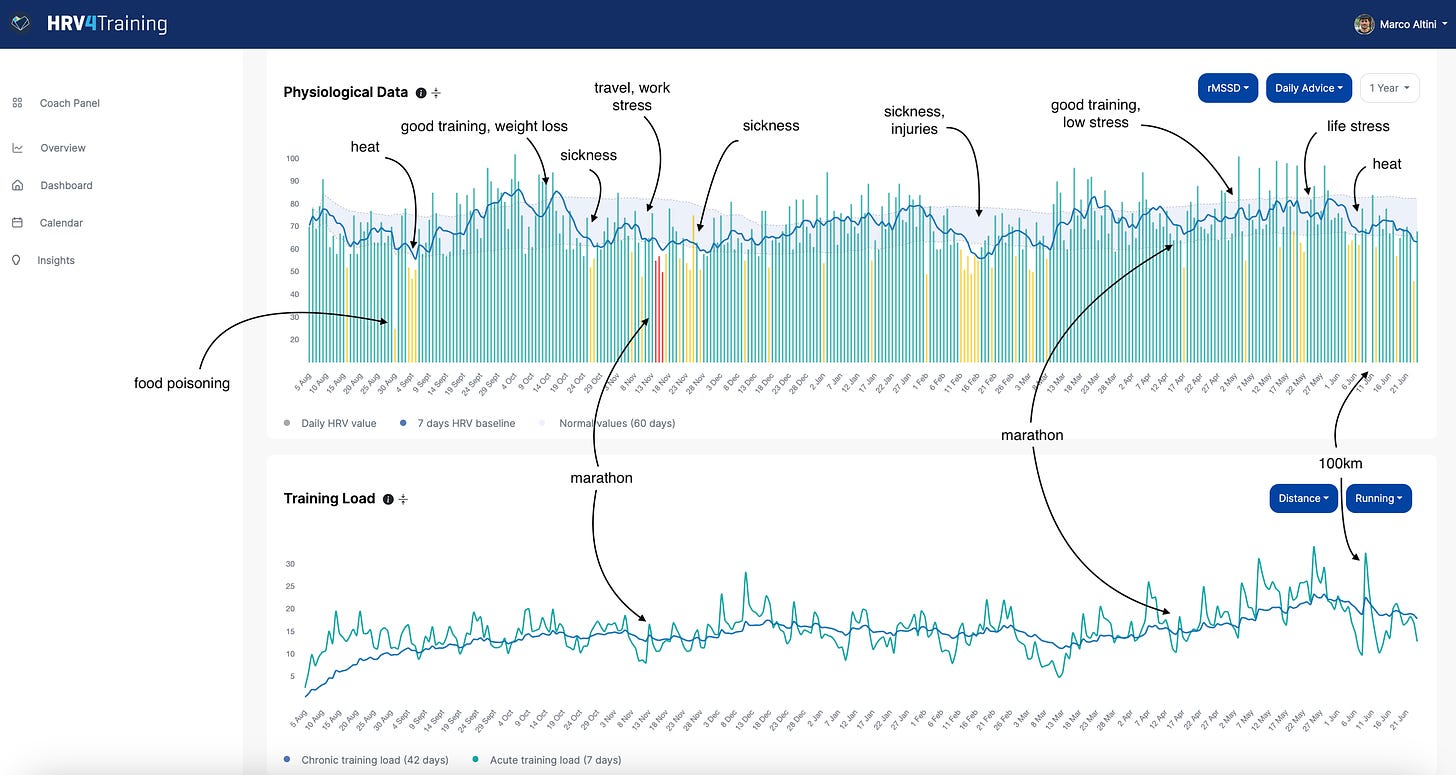
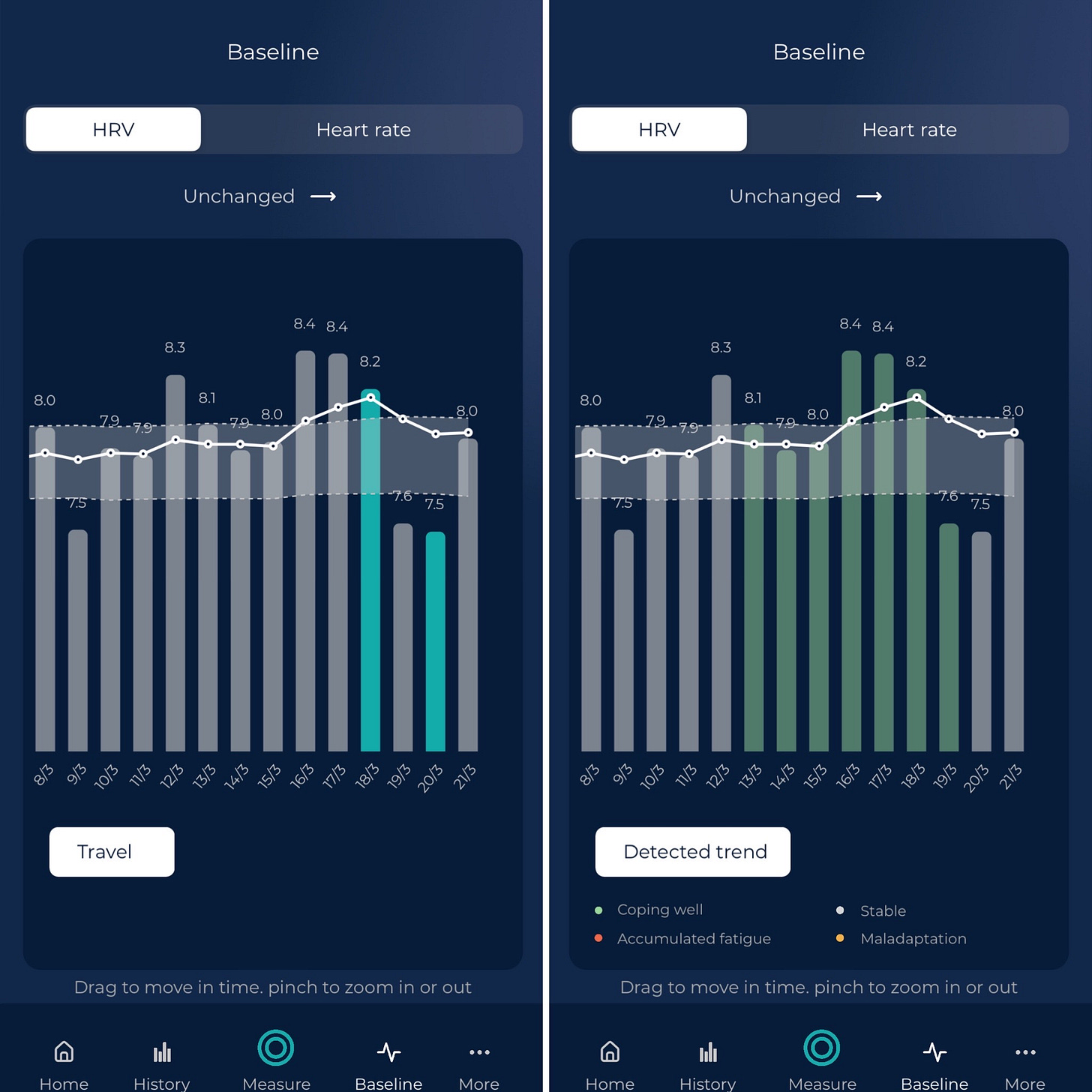
See two examples in HRV4Training using my own data (morning measurements while sitting, the protocol I normally recommend, especially for athletes), in the image above:
left pic: chronic work stress, leading to a baseline (white line) below my normal range. These are situations I try to avoid, as my health and performance are affected negatively
right pic: acute stress due to travel, a daily suppression that bounces back after a day, with no change in the baseline. These can be less concerning, but still signal that something is off, with respect to a more stable profile (my health might be okay, but my performance might not)
I hope this writeup was informative.
Discount for Pro: 20% off 🖥️
HRV4Training Pro is the ultimate platform to help you analyze and interpret your physiological data, for individuals and teams.
You can find a guide here.
Try HRV4Training Pro for free at HRVTraining.web.app or use promo code SCIENCE for 20% off.
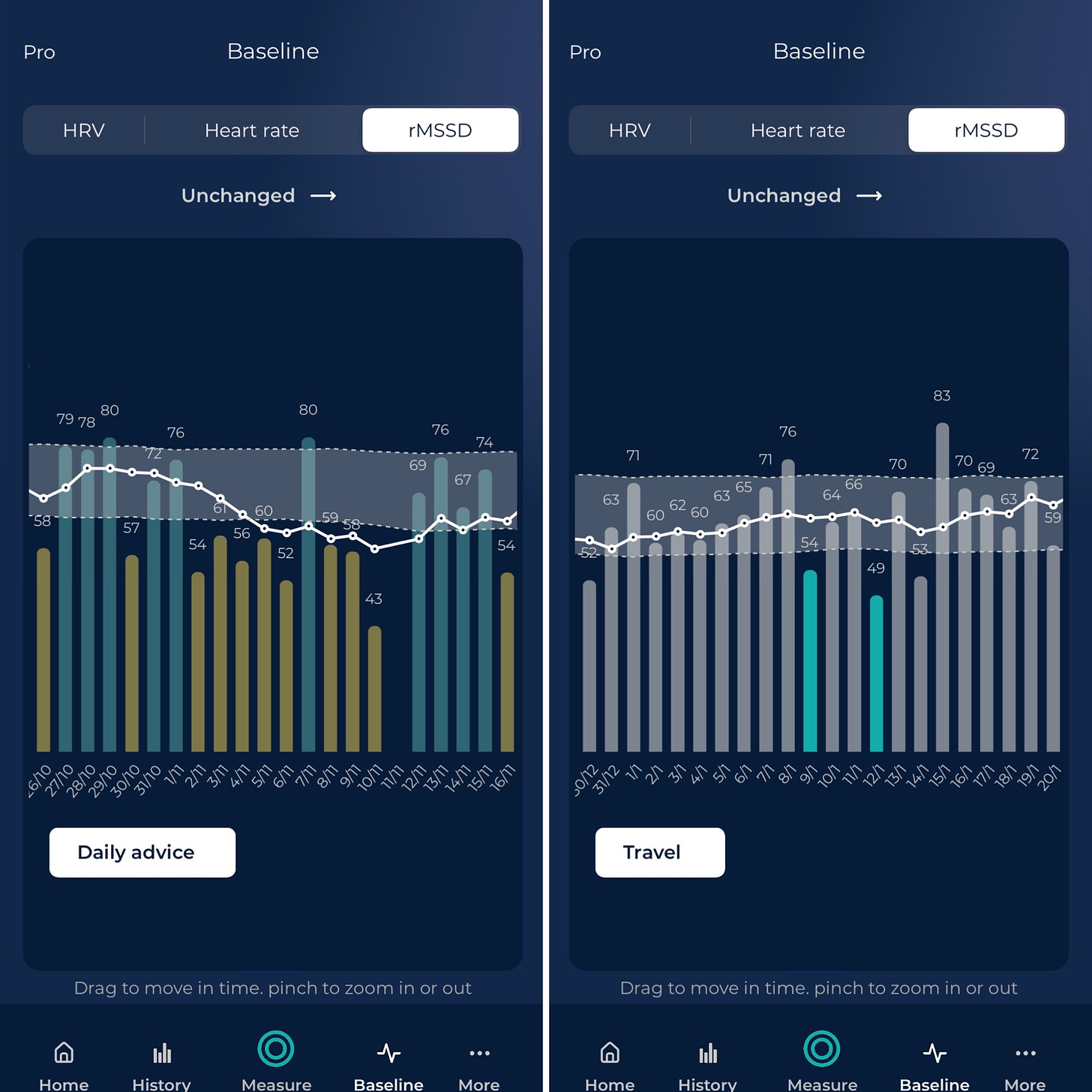
In the app, Pro brings the normal values view, which can help contextualizing longer-term changes, as well as rMSSD on the homepage, see an example below:
See you next week!
Marco holds a PhD cum laude in applied machine learning, a M.Sc. cum laude in computer science engineering, and a M.Sc. cum laude in human movement sciences and high-performance coaching.
He has published more than 50 papers and patents at the intersection between physiology, health, technology, and human performance.
He is co-founder of HRV4Training, advisor at Oura, guest lecturer at VU Amsterdam, and editor for IEEE Pervasive Computing Magazine. He loves running.
Social:
Twitter: @altini_marco.
Personal Substack.





Awesome article, thanks Marco! While I understood the point that HRV shouldn't be used as an outcome measure in itself, I have seen papers that use resonance breathing with HRV biofeedback to help people with medical conditions that have abnormally low HRV (like your biofeedback app - PS would love it on Android!). Would you say that it's use as an outcome measure in these cases are useful or misconception too? In regards to the normal range, does HRV4Training continuously update our normal range as we enter more records or is it based on the first 4 days of use? Cheers!
A really interesting and helpful article 👌